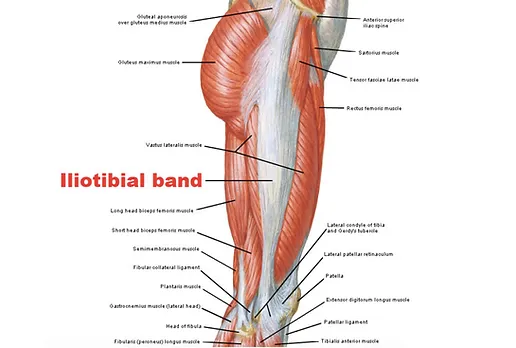
Iliotibial (IT) Band Pain Syndrome is a frequently observed overuse injury in individuals who engage in running, cycling, and various athletic activities. This condition frequently manifests as a sharp discomfort along the outer aspect of the knee and tends to worsen with ongoing and repetitive activity. In some instances, it may also result in a clicking or snapping sensation along the outside of the knee.
Anatomy
The IT band is a connective tissue that runs from the outer hip (iliac crest) and extends down the outer thigh, attaching just below the outside of the knee. It plays a crucial role in providing stability to both the hip and the knee joint.
The IT band serves as an anchor point for several muscular and soft tissue structures, including the tensor fascia lata (TFL), the gluteus medius and maximus, and the vastus lateralis (the outer portion of the quadricep). The well-being and function of all these tissues significantly influences the overall health of the IT band.
What Leads to IT Band Pain?
There are several contributing factors to the development of IT band pain:
Weakness Deficits: Insufficient strength in the glute medius and glute maximus can lead to compromised pelvic control, resulting in instability during activities like squatting, running, and climbing stairs. Weakness in the quadriceps can lead to reduced force absorption, placing additional stress on the knee.
Mobility Deficits — Soft Tissue: Muscle restrictions around or connected to the IT band are common. Key areas to examine are the gluteal muscles, vastus lateralis, TFL, and gastroc. A common issue is an overactive, restricted TFL in combination with an underactive gluteus medius, resulting in hip and knee collapsing mechanics.
Mobility Deficits — Joint: Two joints that can influence IT band symptoms are the patellofemoral joint and the ankle. Inadequate knee cap mobility can restrict knee movement, and limited ankle mobility can alter gait mechanics, leading to increased foot pronation and additional strain on the IT band.
Poor Movement Mechanics: Poor pelvic control can lead to valgus collapse (inward knee drop), while excessive foot pronation can result in valgus collapse from the bottom up.
Running Mechanics: A gait assessment can help identify common deviations that can lead to IT band pain, such as collapsing mechanics, weaving mechanics, and overstriding.
Training Variables: Rapidly increasing training volume, terrain choice (consistently running in one direction on a track), and footwear all influence IT band pain.
Footwear: Wearing worn-out shoes can negatively impact mechanics throughout the chain. Shoes should not be worn beyond 300–500 miles per pair, and it's often recommended to rotate between at least two pairs.
What to Avoid When Dealing with IT Band Pain
It's important to note that none of the previously mentioned causes of IT band pain are related to the flexibility, mobility, or tightness of the IT band itself. Since the IT band consists of fascial tissue, it cannot be stretched or foam rolled, nor can it be strengthened. The approach to alleviating IT band symptoms involves addressing the regions above, below, and connected to it.
How to Effectively Treat IT Band Pain
Start with mobility! If an individual lacks sufficient range of motion in the knee, patellar mobility, or ankle mobility, they are not adequately prepared for strengthening or making mechanical changes.
Enhancing the mobility of tissues through techniques like foam rolling, trigger point release, active release methods, or other soft tissue mobilization can quickly improve the activation and function of these muscles.
The key takeaway is that no amount of strength or gait retraining can compensate for a mobility deficit.
Once mobility has been properly restored, shift your focus to strength. Without adequate strength, the body lacks the stability necessary to control the substantial range of motion required in activities like running and cycling.
Dig deeper! After addressing the fundamental deficits, it's time to concentrate on movement patterns, proper squat mechanics, and gait retraining using movement analysis. This is where you ensure that you are instilling good habits that ideally prevent the pain from recurring.
If you need help dealing with IT band pain, schedule your session with our sports physical therapist.